 15 Their observations do not oppose our findings. Other authors have previously focused on the optical reflectivity of cysts in different retinal diseases, demonstrating that the optical reflectivity could show heterogeneity of reflectivity, especially in DME. 14 The new approach presented here for the first time permits the identification, location, and mapping of areas of fluid accumulation and their correlation with changes in RT. Previous attempts to identify sites of LOR in the OCT, with changes in the spaces between cells, and to correlate them with sites of BRB breakdown have demonstrated only limited utility. They were gathered using a licensed feature that exports 8-bit binary data for research purposes. The data were processed by using the 8-bit reduced data set of the Zeiss Cirrus 5000. Only scans with signal strength of 7 and above were considered. The data were exported using a licensed feature of the Cirrus that exports 8-bit binary data for research purposes. We used the 8-bit reduced dataset of the Zeiss Cirrus 5000. The threshold was chosen considering the full retina scan and represents a value set below the mean plus 2 standard deviations of the value obtained in the healthy control eyes. The threshold value is established for the OCT device used, as it is dependent on the equipment ( Fig. To be able to identify abnormal increases in extracellular space, we first established a threshold value for optical reflectivity from A-scans obtained from a series of healthy control eyes using HD-OCT Cirrus 5000. 
Therefore, it is considered that retinal extracellular fluid distribution will be identified by sites of low OCT optical reflectivity. 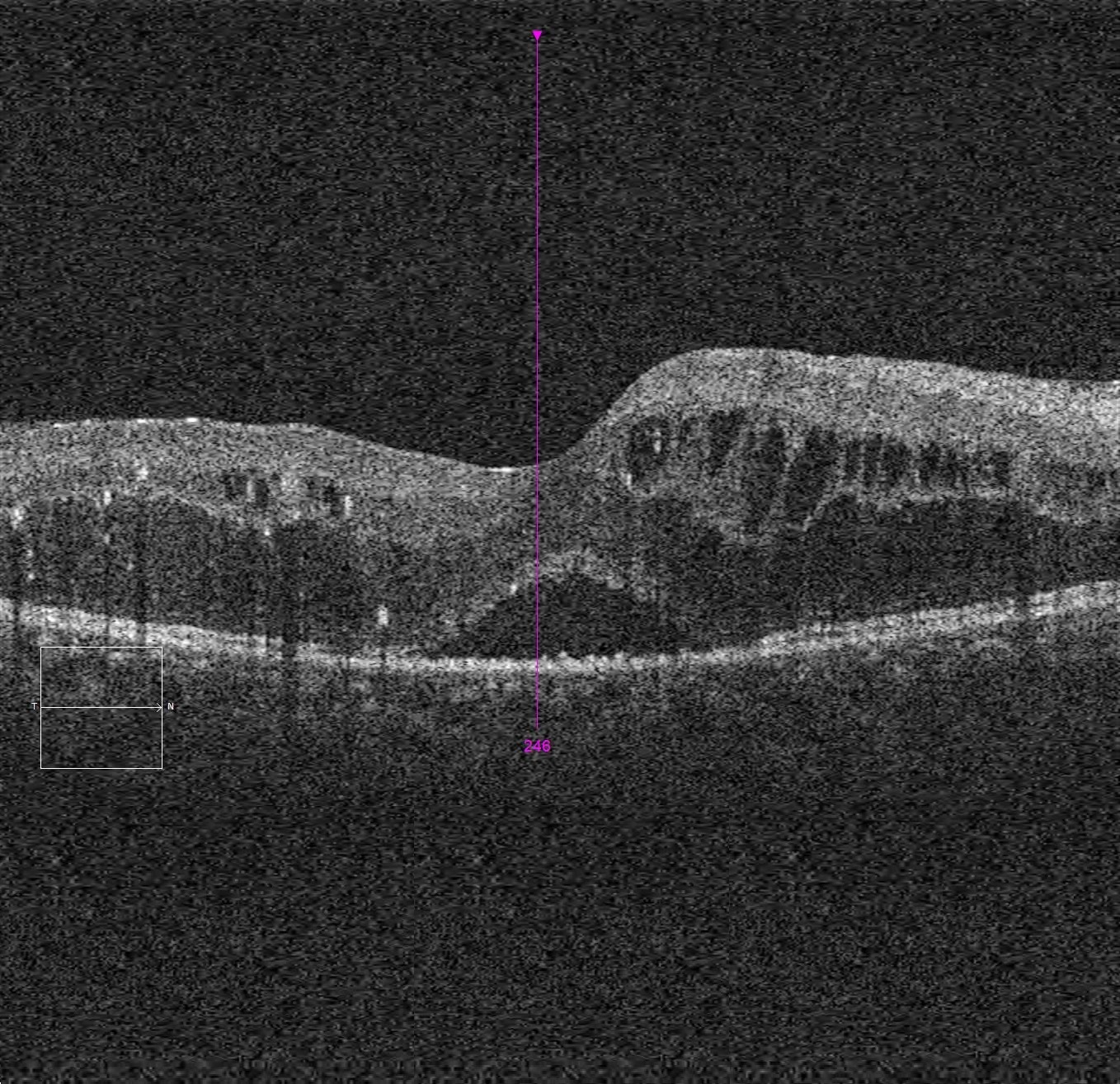
Diabetic macular edema is represented mainly by extracellular fluid accumulation that preferentially involves the INL of the retina.Ĭell nuclei in the retina have higher reflectivity than water-filled areas. 
Increases in number of sites with lower optical reflectivity positively correlate with the increase in RT in the initial stages of macular edema in diabetes type 2. Extracellular space increases in the INL that were identified with the OCT-Leakage algorithm showed a strong positive correlation with the increases in RT in the central subfield ( r = 0.71, P < 0.001). These increases were, on average, 49.9% in subclinical macular edema and 104.7% in clinical macular edema. The highest increases in RT in the eyes with subclinical and clinical macular edema were found in the inner nuclear layer (INL). Results from automated analysis of the retinal extracellular space, using our OCT-Leakage algorithm to identify sites of low optical reflectivity, were compared with those from a control group of 25 healthy eyes. They were examined with Cirrus spectral-domain optical coherence tomography (OCT) at baseline visits ( number, NCT01145599) in the Coimbra center. To identify retinal extracellular fluid changes and their correlation with increased retinal thickness (RT) in eyes with subclinical and clinical macular edema in diabetes type 2.Ī cohort of 48 eyes from 48 type 2 diabetic patients with mild or moderate nonproliferative diabetic retinopathy (Early Treatment Diabetic Retinopathy Study levels 20/35) were classified as having normal RT (10), subclinical macular edema (30), or clinical macular edema (8). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
